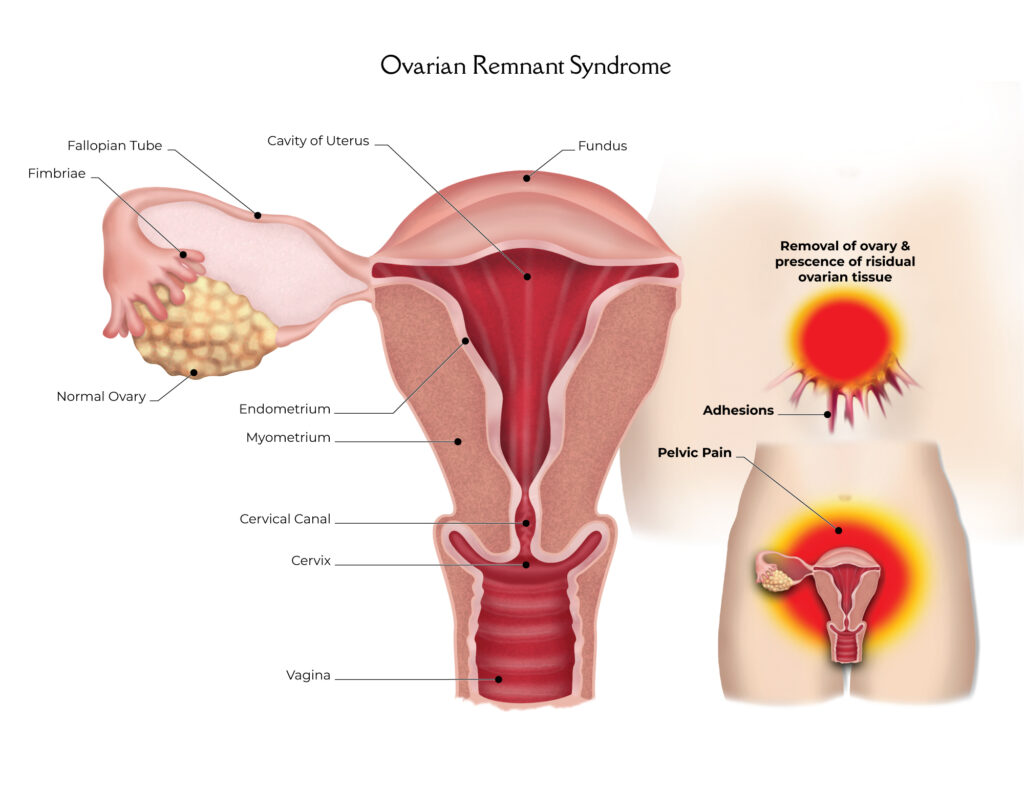
Ovarian Remnant Syndrome (ORS) is a relatively rare but significant condition that affects women who have undergone a complete hysterectomy or oophorectomy (removal of the ovaries). Despite these surgeries, small pieces of ovarian tissue can remain in the pelvic cavity, leading to persistent or recurring symptoms. This article aims to provide a comprehensive overview of how ORS occurs, its symptoms, and the available treatment options.
How Does Ovarian Remnant Syndrome Occur?
Ovarian Remnant Syndrome occurs when ovarian tissue is inadvertently left behind during surgery. The following factors contribute to the development of ORS:
- Technical Challenges During Surgery: The pelvic region is a complex area with many vital structures. Removing the ovaries entirely can be technically challenging, especially if there are adhesions (scar tissue) from previous surgeries or conditions like endometriosis. These adhesions can make it difficult for surgeons to access and remove the ovaries completely.
- Microscopic Ovarian Tissue: During surgery, microscopic fragments of ovarian tissue may not be visible to the naked eye. These tiny fragments can remain in the pelvic cavity and later grow and function as ovarian tissue, leading to ORS. Even the most meticulous surgical techniques can leave behind these small remnants.
- Adhesions and Scarring: Adhesions can obscure ovarian tissue, making it more likely that some remnants are left behind. Scar tissue can also complicate the surgical procedure, increasing the risk of incomplete removal of the ovaries.
- Incomplete Oophorectomy: In some cases, an oophorectomy may be intentionally incomplete to avoid damaging nearby organs or blood vessels. While this approach can be necessary to ensure patient safety, it can also increase the risk of ORS.
- Surgeon Experience and Technique: The skill and experience of the surgeon play a critical role in the success of the procedure. Surgeons with less experience in complex pelvic surgeries may have a higher likelihood of leaving behind ovarian remnants.
Symptoms of Ovarian Remnant Syndrome
The symptoms of ORS can vary widely among individuals, but they often mimic those of ovarian cysts or other ovarian disorders. Common symptoms include:
- Pelvic Pain: Persistent or intermittent pelvic pain is the most common symptom of ORS. The pain can be similar to that experienced before the ovaries were removed and may worsen during certain activities or menstrual cycles.
- Pelvic Mass: A pelvic mass or lump may be detectable during a physical examination or imaging studies. This mass is often caused by the growth of ovarian tissue remnants.
- Menstrual Irregularities: In women who have not undergone a complete hysterectomy, menstrual irregularities or the return of menstrual periods can occur. This is due to the residual ovarian tissue continuing to produce hormones.
- Hormonal Symptoms: Symptoms related to hormonal activity, such as breast tenderness, mood swings, or hot flashes, may be present if the remaining ovarian tissue is still functional. These symptoms can be confusing and distressing for women who believed they were entering menopause.
Diagnosis of Ovarian Remnant Syndrome
Diagnosing ORS can be challenging due to the non-specific nature of its symptoms. A combination of medical history, physical examination, and imaging studies (such as ultrasound, CT scan, or MRI) is typically used to identify the presence of residual ovarian tissue. However, imaging alone may not always be sufficient, as small remnants can be difficult to detect.
Medical History: A detailed medical history is crucial for diagnosing ORS. Patients should provide information about previous surgeries, including the type of surgery, the reason for the surgery, and any complications that occurred.
Physical Examination: A pelvic examination can help detect the presence of a pelvic mass or tenderness in the affected area. However, physical examinations alone are often inconclusive.
Imaging Studies: Imaging studies such as ultrasound, CT scan, or MRI can help visualize the pelvic cavity and identify any remaining ovarian tissue. However, these imaging techniques may not always detect small remnants, making the diagnosis challenging.
Hormonal Tests: Hormonal tests can help determine if the remaining ovarian tissue is still functional. Elevated levels of hormones such as estrogen and progesterone may indicate the presence of functioning ovarian remnants.
Treatment of Ovarian Remnant Syndrome
Treatment for ORS typically involves a combination of medical and surgical approaches, depending on the severity of symptoms and the individual patient’s circumstances. The goal of treatment is to alleviate symptoms, manage pain, and address any hormonal imbalances.
Medications: Hormonal therapies, such as gonadotropin-releasing hormone (GnRH) agonists, may be used to suppress ovarian function and alleviate symptoms. These medications work by reducing the production of hormones that stimulate ovarian tissue growth. Pain medications, including nonsteroidal anti-inflammatory drugs (NSAIDs) and opioids, may also be prescribed to manage chronic pelvic pain.
Surgery: Surgical removal of the remaining ovarian tissue is often necessary to provide relief from symptoms. This procedure, known as “re-exploration surgery,” can be challenging and may require a highly skilled surgeon with experience in complex pelvic surgeries. The success of surgery depends on the surgeon’s ability to locate and remove all remaining ovarian tissue.
Pain Management: Pain management strategies, including medications, physical therapy, and other non-surgical interventions, may be recommended to manage chronic pelvic pain. Pain management specialists can work with patients to develop a comprehensive plan that addresses both acute and chronic pain.
Hormonal Suppression: Hormonal suppression therapy can help manage symptoms by reducing the activity of the remaining ovarian tissue. This approach may involve the use of oral contraceptives, GnRH agonists, or other hormonal medications.
Coping with Ovarian Remnant Syndrome
Living with ORS can be challenging, but support and understanding from healthcare providers, family, and friends can make a significant difference. Women with ORS should work closely with their healthcare team to develop a comprehensive treatment plan tailored to their specific needs.
Education and Awareness: Education about ORS is essential for both patients and healthcare providers. Understanding the condition, its symptoms, and available treatment options can empower women to make informed decisions about their care.
Regular Follow-Up: Regular follow-up appointments with healthcare providers are crucial for monitoring symptoms and assessing the effectiveness of treatment. Ongoing communication with the healthcare team can help address any concerns or changes in symptoms.
Support Groups and Counseling: Support groups and counseling can provide emotional support and practical advice for those affected by ORS. Connecting with others who have experienced similar challenges can help reduce feelings of isolation and provide valuable insights into coping strategies.
Conclusion
Ovarian Remnant Syndrome is a rare but significant condition that can cause persistent pain and other symptoms in women who have undergone oophorectomy or hysterectomy. Understanding how ORS occurs, recognizing its symptoms, and seeking appropriate medical care are crucial steps in managing this condition effectively. With the right treatment and support, women with ORS can lead healthy, fulfilling lives. If you suspect you may have ORS, it is important to consult with a healthcare provider who can guide you through the diagnostic process and develop a personalized treatment plan.
Stay tuned for more news and updates on Infinite Insight Hub!